Some Employees May Face COVID-19 Health Insurance Surcharges
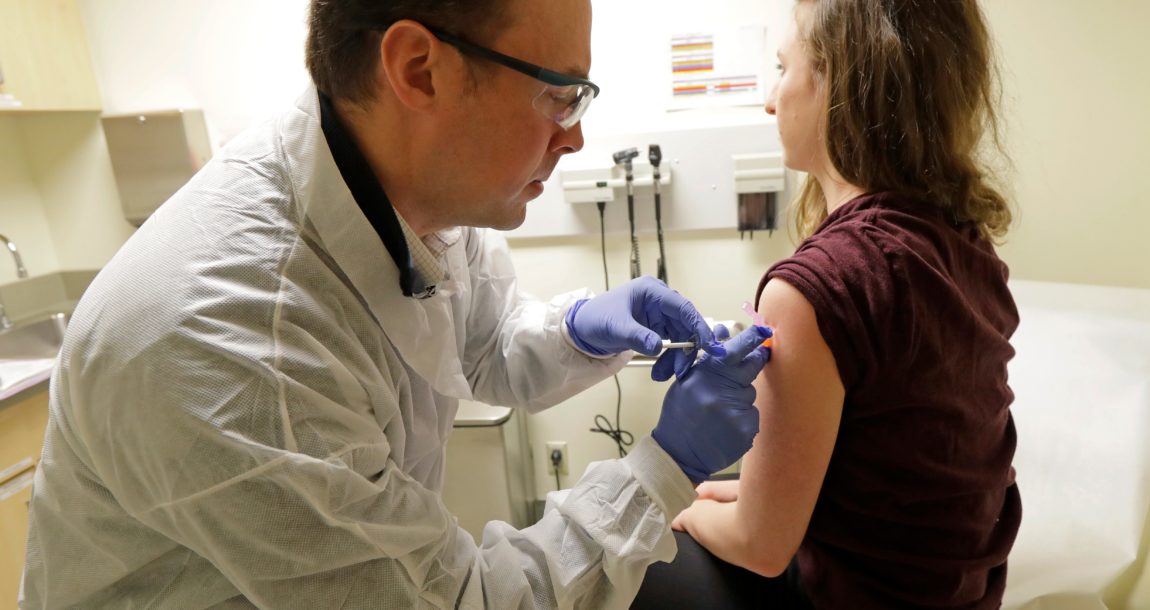
An announcement Wednesday by Atlanta-based Delta Air Lines that it will charge a monthly surcharge for employees who have not been vaccinated against COVID-19 may be a harbinger of things to come.
But, in Washington, employees in companies that do not self-insure are unlikely to face such additional fees.
According to Stephanie Marquis, a spokesperson for Washington state Office of the Insurance Commissioner, which oversees state health insurance plans, the insurance companies that provide health care coverage for many companies and their employees cannot impose such fees.
"That's not allowed in state-regulated plans," Marquis said.
In a statement issued Wednesday morning, Delta CEO Ed Bastian said as of Nov. 1, the company will charge all unvaccinated employees an additional $200 per month, noting every Delta employee hospitalized with COVID-19 has cost the airline an average of $50,000 per stay and that "all Delta employees who have been hospitalized with COVID were not fully vaccinated."
Marquis said as a large employer — Delta has roughly 68,000 employees — the airline does not purchase health insurance from a company like Blue Cross or Aetna, but self-insures, setting aside employee premiums and company contributions in a separate fund to pay for health care.
"For the self-insured, that's allowed, they are outside of state regulations," she said. "And that's who you will see do it."
"We are not implementing or considering surcharges for our members who are unvaccinated," wrote Courtney Wallace, the director of strategic communications for Premera, a Blue Cross Blue Shield affiliate in Washington, in an email to the Columbia Basin Herald.
Premera is the largest group health insurance provider in Washington in 2020, according to a report from the Office of the Insurance Commissioner, with more than 333,000 enrolled members, comprising 22% of the state's group health insurance market.
According to a Kaiser Family Foundation on employer-provided health insurance published in October 2020, employer health insurance plans cover approximately 157 million people in the United States, with 67% of those covered by self-insured plans. The bulk of companies covered by self-insured plans, 84%, are large firms with 500 or more employees, the report said.
In addition, most health insurers have stopped waiving co-pays for COVID-19-related treatment costs, a practice enacted at the beginning of the pandemic but only covered by law or formal agreement in a handful of states. A separate Kaiser Family Foundation study published this month found that 72% of the largest health insurers in the U.S. have stopped waiving co-pays for COVID-treatment, and another 10% are expected to soon.
"Waivers for COVID-19-related treatment, which included co-pays, deductibles and co-insurance, ended on June 30, 2021," Wallace wrote.
Wallace said Premera is still covering COVID-19 treatments as part of its members' policies, but it is "only the cost share that has ended."
Marquis said by law, the only COVID-19-related co-pays insurers are required to waive are for tests, and she said most insurers at this point have stopped waivers for treatment co-pays.
___
(c)2021 the Columbia Basin Herald, Wash.
Visit the Columbia Basin Herald, Wash. at www.columbiabasinherald.com
Distributed by Tribune Content Agency, LLC.




$14.3 million project to help Highland neighborhood flooded in 2010
N.H. Insurance Department's Consumer Services Unit Delivers Results for Granite Staters in FY 2021
Advisor News
- Charitable giving tools available for taxpayers; due to expire
- Study: How should lawmakers fix the Social Security gap?
- Could Trump seek revenue via a sharp cut in 401(k) contribution limits?
- The ‘guardrails approach’ to retirement income
- Is there a mismatch between advisor marketing and consumer preferences?
More Advisor NewsAnnuity News
Health/Employee Benefits News
- Best’s Market Segment Report: US Health Insurers Met Challenges in 2024 but Pressures Expected to Persist in 2025
- What They're Not Telling You About Farm Bureau Health Plans
- Many are confused over their health plan design
- Medicaid caps could cost states $1.1 trillion
- ‘It is, frankly, dangerous’: Addiction treatment centers claim insurance denials have increased
More Health/Employee Benefits NewsLife Insurance News
- Unum Group Announces $3.4 Billion Long-Term Care Reinsurance Transaction with Fortitude Re
- Insurance Companies
- Zim's Insurance Market Value Seen At U.S.$2,51bn
- Presentation FY 2024
- Somerset Re Accelerates Growth with Strong Deal Momentum into 2025
More Life Insurance News